Treatments Not to Use
There are many treatments that people will recommend that do not help angular cheilitis and in many cases it can make it more painful or worse. This page will go over the treatments that you should not use and habits you should break when you have angular cheilitis.Touching Your Mouth
 It's a fairly common habit for people to touch their mouths when thinking, resting their head, etc. However, you should try to keep yourself from touching your lips when you have angular cheilitis. The reason is because our hands and fingers are extremely dirty and angular cheilitis causes open wounds on your mouth. So every time you touch your mouth with dirty finger you are potentially introducing new bacteria to area making it more difficult for your body to heal itself. If you must touch your lips, be sure to thoroughly wash your hands before you do so.
It's a fairly common habit for people to touch their mouths when thinking, resting their head, etc. However, you should try to keep yourself from touching your lips when you have angular cheilitis. The reason is because our hands and fingers are extremely dirty and angular cheilitis causes open wounds on your mouth. So every time you touch your mouth with dirty finger you are potentially introducing new bacteria to area making it more difficult for your body to heal itself. If you must touch your lips, be sure to thoroughly wash your hands before you do so.
Frequently Picking At Your Wounds
 Yes, when your angular cheilitis begins to heal it looks gross and unattractive. However, your hands are dirty so you should try your best to not touch your wounds. Normally the best way to get rid of the gross crust and flaky skin is to wash your hands, get a warm washcloth, and gently rub it away. If you have angular cheilitis in both corners of your mouth be sure to use a different wash cloth before cleaning the other side to prevent spreading the bacteria across your mouth.
Yes, when your angular cheilitis begins to heal it looks gross and unattractive. However, your hands are dirty so you should try your best to not touch your wounds. Normally the best way to get rid of the gross crust and flaky skin is to wash your hands, get a warm washcloth, and gently rub it away. If you have angular cheilitis in both corners of your mouth be sure to use a different wash cloth before cleaning the other side to prevent spreading the bacteria across your mouth.
Bleach (Peroxide) for Angular Cheilitis
 Bleach is an extremely corrosive chemical that will irritate skin, eyes, and your respiratory system. Toxic exposure to bleach has been linked to many life-long health issues. Many hospitals and doctors offices may use wound cleaners with a partial-bleach base to treat serious wounds, however this does not mean it should ever be used for medical purposes at the home other than disinfecting cleaning utensils and clothing.
Bleach is an extremely corrosive chemical that will irritate skin, eyes, and your respiratory system. Toxic exposure to bleach has been linked to many life-long health issues. Many hospitals and doctors offices may use wound cleaners with a partial-bleach base to treat serious wounds, however this does not mean it should ever be used for medical purposes at the home other than disinfecting cleaning utensils and clothing.
Chapstick for Angular Cheilitis
Usually when people have angular cheilitis they also have chapped lips, so it's not uncommon for people to use chapstick frequently for relief. However, chapstick can make angular cheilitis worse if used incorrectly. If you need to use chapstick be sure to follow these two rules:
Do not use hard chapstick from a tube. Instead, use soft lip-balm. Tube chapstick requires more pressure to spread it across your lips, plus it spreads the angular cheilitis bacteria and fungus across your entire mouth before sealing it into the chapstick tube. If you're using chapstick from the tube, you will either want to thoroughly clean it or throw it away and get some new chapstick.
 To prevent contaminating the chapstick/lip-balm you will need to apply the balm to your lips with clean fingers. Get enough of the balm on your finger that you don't have to re-apply it to your finger after you touch your lips (if you need to do this, use a different finger or wash your hands before doing so). When applying it to your lips, start in the middle of your lip and work towards your mouth corners. This way you will end at your mouth corner which prevents you from spreading the angular cheilitis bacteria and fungus across your mouth.
To prevent contaminating the chapstick/lip-balm you will need to apply the balm to your lips with clean fingers. Get enough of the balm on your finger that you don't have to re-apply it to your finger after you touch your lips (if you need to do this, use a different finger or wash your hands before doing so). When applying it to your lips, start in the middle of your lip and work towards your mouth corners. This way you will end at your mouth corner which prevents you from spreading the angular cheilitis bacteria and fungus across your mouth.
This same rule applies for all other balms you put on your lips including lipstick, gloss, etc.
 Cold Sore Medications for Angular Cheilitis (Abreva, Campho-phenique, etc.)
Cold Sore Medications for Angular Cheilitis (Abreva, Campho-phenique, etc.)Many people think they have angular cheilitis when they actually have a cold sore. So they will oftentimes swear that cold sore medications work. However, they do nothing for angular cheilitis. In fact, most cold sore medications contain a drying agent which may dry the skin on your lips even more.
Humidifier for Angular Cheilitis
Humidifiers are used to increase the humidity of a room. However, angular cheilitis does not need any additional moisture since it is constantly in contact with the saliva from our mouth.
Neosporin for Angular Cheilitis
 Neosporin is intended to treat minor cuts, scrapes, and burns and should not get in your mouth. Angular cheilitis is a bacterial/fungal infection on very close to your mouth. The only positive use Neosporin should have for angular cheilitis is it can help to prevent scarring on the outside of your mouth in cases where the lesions become severe and split.
Neosporin is intended to treat minor cuts, scrapes, and burns and should not get in your mouth. Angular cheilitis is a bacterial/fungal infection on very close to your mouth. The only positive use Neosporin should have for angular cheilitis is it can help to prevent scarring on the outside of your mouth in cases where the lesions become severe and split.
 Learn how to treat angular cheilitis, including home remedies, over the counter treatments, and more.
Learn how to treat angular cheilitis, including home remedies, over the counter treatments, and more. « Go to The Previous Page

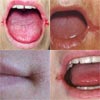 View pictures of people who have angular cheilitis so you can see if it resembles what you have.
View pictures of people who have angular cheilitis so you can see if it resembles what you have.